The hormonal contraceptive coil (LNG-IUD)

The hormonal coil (LNG-IUD)
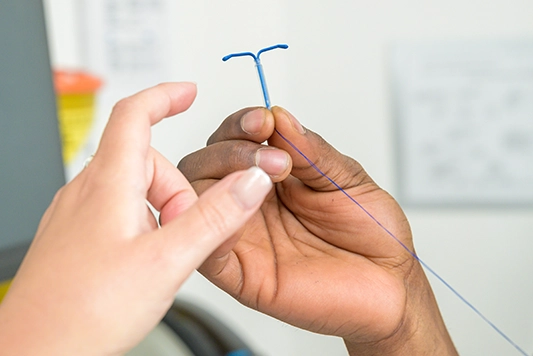
The hormonal coil (also known by multiple brand names such as “Mirena”, and formerly known as the IUS) is a small T-shaped plastic device that is fitted in the uterus (womb). It provides contraceptive protection for up to eight years.
The hormonal coil steadily releases small amounts of a hormone called progestogen which thickens the fluid around the neck of the uterus (stopping sperm from getting to an egg) and makes the lining of the uterus thinner so that a fertilised egg cannot grow.
Video – the hormonal coil
Would you like to find out everything you need to know about the hormonal coil in under two minutes? We’ve created this short explainer video, filled with information about the hormonal coil including:
– What it is and how it works
– How effective it is in protecting against pregnancy
– Advantages
– Disadvantages
– Risks

Getting the hormonal coil fitted
Inserting a hormonal coil is a simple procedure that takes about 5 minutes. A trained person inserts the coil through the vagina. The hormonal coil sits in the uterus and does not move from there.
There are threads attached to the hormonal coil which sit in the vagina that assist with removal and allow you and your provider want to check the coil is in the right place.
It is rare for the hormonal coil to fall out or move. Most people can self-examine and feel the small, very thin thread attached to the end of the coil which comes out of the cervix and into the vagina. When you have the coil inserted make sure your healthcare provider shows you how to find the thread so you feel confident to find it again.
How might the hormonal coil affect my hormones?
Whilst the hormonal coil releases a hormone called progesterone, this hormone is localised, and so it is less likely that you’ll experience the same sorts of side effects associated with combined contraceptive methods like the combined pill, patch or ring. Additionally, there are different doses of hormones in different types of hormonal coil – for example, the Mirena coil and Levosert has a higher dose than the Kyleena coil.
How might the hormonal coil affect my periods?
Whilst the non-hormonal coil (also known as the copper coil) might exacerbate heavy or painful periods, the hormonal coil might be recommended to support with heavy periods.
How effective is the hormonal coil?
The hormonal coil works very well at preventing pregnancy.
The hormonal coil is more than 99% effective. Fewer than 1 in 100 people will get pregnant over the 3 to 8 years when using an hormonal coil.
How long does it take for the hormonal coil to work?
If the hormonal coil is fitted during the first five days of your menstrual cycle, you’ll be immediately protected against becoming pregnant. If it’s fitted on any other day of your menstrual cycle, you’ll need to use additional contraception (such as condoms) for seven days.
Coil fitting and pain management
The experience of having intrauterine contraception (such as the hormonal coil or non-hormonal coil) fitted differs from person to person.
The most important thing to remember is that you can ask for pain relief. At MSI Reproductive Choices, we offer anyone opting for a coil a choice of four types of local anaesthetic, including: an anaesthetic gel, spray, an injection and a cream, as well as suggesting the option of taking painkillers, such as ibuprofen, an hour or two before the procedure. Each of these methods of anaesthetic are applied to the cervix (the injection, for example, is applied inside the cervix), and you can choose to have more than one method of anaesthetic if the initial method you use isn’t easing your pain. There is no recovery time for this anaesthetic, and so it is safe for you to drive after your appointment. If you are having your coil fitted or removed with another provider, you may want to ask whether pain relief is provided when you book your appointment.
These anaesthetics may not completely take away the discomfort, and there may still be cramping pain after the fitting (this may last for up to a couple of days).
It’s always good to have something to eat before a coil fitting appointment in case you feel faint at any point, and to wear clothes that are comfortable and easy to change in or out of.
Remember that you are in control, and that you can stop or take a break at any point if you want to. You can also ask to have a chaperone or another healthcare practitioner with you during your appointment, to support you and ensure you feel comfortable throughout.
Other LARC methods
Follow the links below to find information about other long-acting reversible contraceptive methods.

The contraceptive injection
Find all you need to know about the contraceptive injection.

The non-hormonal coil (CU-IUD)
Find all you need to know about the non-hormonal coil (also known as the copper coil).
The contraceptive implant
Find all you need to know about the contraceptive implant.
Advantages, disadvantages, side effects and risks associated with the hormonal coil
Once in place, you don’t need to think about the hormonal coil or do anything until it needs replacing, which can be up to eight years, depending on the type of hormonal coil you are using.
You can get the coil removed whenever you want.
Your fertility will return to normal immediately after the hormonal coil is removed.
The hormonal coil is great if you have heavy or painful periods, as it usually makes periods lighter and less painful. Many users stop getting periods with the hormonal coil. Lighter or no monthly bleeding is not harmful and will not affect future fertility.
The hormonal coil can be inserted right after childbirth, abortion or miscarriage.
It is not used during sex so will not affect spontaneity. Neither you nor your partner should be aware of the coil during sex.
A hormonal coil requires a vaginal examination and a simple, short procedure to fit it in the uterus (womb).
The most common side effects of the hormonal coil are lighter and fewer days of bleeding, or irregular bleeding. Many users stop having a monthly period. Irregular bleeding or spotting should settle within the first six months of use.
A small number of users may experience other side effects due to the hormone in the hormonal coil, such as acne, headaches, or breast tenderness. These usually settle down after the first few months of use.
Condoms are the only contraceptive method which protect against sexually transmitted infections. To ensure protection from both pregnancy and infection, we recommend “dual protection”. This means using a male or female condom in addition to the contraceptive method of your choice to prevent pregnancy.
There is a small risk of infection when the hormonal coil is put in.
There’s a very small risk that the coil might go through (perforate) your uterus (womb) or cervix when it’s put in. If it does happen, the coil may have to be removed by surgery.
If the coil moves out of place or falls out, it can stop providing protection against pregnancy.
Where can I book an appointment for hormonal coil fitting and removal?
In the UK, you can make an appointment to have the hormonal coil fitted or removed – and to access other LARC (Long-Acting Reversible Contraception) services, such as implant fitting and removal – at sexual health clinics, contraception clinics and some GP surgeries.
At MSI UK, we primarily offer contraception services as part of your abortion care. We also offer contraception services in some parts of England for people who have not accessed our abortion services. From these clinics, people can access LARC (Long-Acting Reversible Contraception, such as the coils, the implant and the injection) with us without having had an abortion.
Follow the link to find out more: MSI UK Contraception Clinics
Having the hormonal coil fitted as part of abortion care with MSI UK
As part of NHS-funded abortion care, we offer a range of contraception methods should you wish to start a method at the time of your treatment.
If you are having a surgical abortion with MSI UK, we can arrange for the hormonal coil to be fitted during or on the same day as your abortion treatment.
If you have a medical abortion (including telemedicine), a nurse will be able to arrange an appointment for you to have the hormonal coil fitted following your abortion.
Learn more about contraception
Visit the pages below to find a comparison tool to help you find the right method for you, to learn more about long-acting reversible contraception and to find information about MSI UK’s contraception clinics.

Which method is right for me?
Find a contraception comparison tool that can help you find the right method for you.

MSI UK contraception clinics
Here, people can access long-acting reversible contraception without having had an abortion.

Long-acting contraception
Long-acting contraceptive methods include the coils, the injection and the implant.

